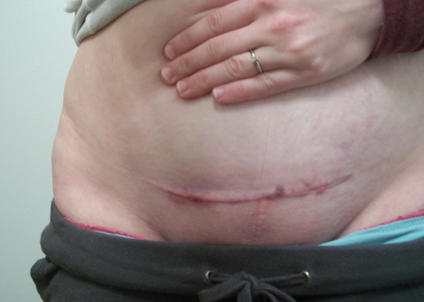
After a very inspiring discussion with Jay Duncan of VIDA doulas, I became acutely aware of a lack of information given to women who have delivered via C-section that teaches them to care for their incision and optimize healing. There is a lot of discussion of what ‘not-to-do,’ and much of the learning during the post-partum phase seems to focus on infant care and breast health. I would like to share the routine that I give my clients who’ve had a C-section to help them with pain management and set them up for optimal healing.
The two factors I believe impact healing the most are 1) inflammation and 2) swelling. If these two elements are well controlled, then healing is likely to be quick and the outcome should be positive. Prolonged inflammation and swelling can lead to tissue damage and over-production of collagen which results in excess or fibrous scar tissue formation. Remember that it is not just the visible skin that is healing after a caesarian, but the layers of fascia, capillary, muscle and uterine organ tissue below that have to heal as well. The goal is to have each of these layers form a scar that is mobile so that one area is able to move independently of the tissue above and below.
During the first 0-3 weeks post c-section, I recommend that women lie on their back with a couple of pillows underneath their knees and lower legs to elevate them. Next, apply a covered ice pack directly over the incision area and leave on for 10-15 minutes. After that time, remove the ice pack for 45 to 60 minutes to allow the area to return to body temperature, and then re-apply the ice for another 10-15 minutes. This helps manage pain, and causes the blood vessels in the area to act like a pump. When ice is on, the vessels shrink and divert blood, fluid and inflammatory products away from the wound. As the tissue warms again, they open and bring fresh blood to the area. When the ice is placed back on, the vessels shrink again and pump away more fluid; working like a little vacuum. You can repeat this cycle as many times per day as you desire, or have time for.
While in this same position, I encourage women to do some gentle self-manual lymph drainage (MLD). With the finger pads of both hands, slowly and gently press down then release the abdominal tissue below the belly button just enough to move the skin. Working from the midline out to the left side, then from the midline out to the other, do 10-15 slow pumps on each side. Next, locate the center of both inguinal creases (where your upper thigh meets your torso), about two inches down and inwards from the point of your hip bones. Please be careful as this can be close to the incision site. Gently and rhythmically press down then release over the area 30-50 times. MLD is done using only the pressure of a coin on the skin at the frequency of 1 pump every 1-2 seconds. It is a technique that uses light pressure, in a similar way as using ice, to pump fluid away from a wound and return it to the body’s core so it can be eliminated. For a video of Heather Wibbles doing this self-MLD sequence, click here and watch from the 2:36 minute mark to the 4:32 mark.
From 4-6 weeks, women can begin to do some indirect stretching of the tissue in the area surrounding the incision. This will help the collagen fibers within the scar to align themselves in the same direction instead of making a sticky web. “Consolidation” is the term used to describe when the edges of a wound have fused completely and a scar is strong enough to resist tearing. Full scar consolidation doesn’t happen until the 6 week mark after surgery. Until this time, we must be careful to protect the fusing edges of a scar if there is any strain on the area. To indirectly stretch the scar, I recommend women again lie down on their backs with pillows underneath their knees and lower legs. Starting on the left side of the scar and using the outside border of one hand (the edge near the pinky finger), gently but firmly press down on the tissue just below the incision site to stabilize the scar. While holding that hand in place, use the outside border of the other hand to press down gently and stretch the skin of the abdomen below away from the stabilizing hand. Hold for 20-30 seconds, slowly release, and continue the pattern of stabilizing with one hand while stretching with the other as you work to the right side. Lift both hands up and repeat the same process just above the scar. It is normal to feel some slight discomfort, mild burning, tingling or a pins-and-needles sensation while doing this, but you should NOT feel pain. If you do feel pain, stop and consult with your doctor, midwife or massage therapist.
Provided you have not experienced any complications from infection, after 6 weeks, your RMT will be able to work directly over and with the scar. He or she may do massage, cross fiber frictions, myofascial release, or visceral manipulation, depending on what your needs are. While Massage Therapists can help to mobilize existing scar tissue, the goal is to see your RMT as close to the 6 week mark as possible so that they are able to prevent any adhesions or restrictions from forming in the first place. For more information, please visit my Post Partum Massage page, or contact me, and feel free to book a massage appointment so that we can begin your path to wellness!